Transform Rural Care with Continuous Patient Monitoring
Scalable continuous monitoring that extends high-quality care to remote communities
Rural Monitoring Solutions and Support for LOI and RFP
Whether you’re drafting a Rural Health Transformation (RHT) letter of intent (LOI) or request for proposal (RFP)—or responding to one—we partner with you to design scalable continuous monitoring programs that extend high‑quality care to remote communities and are realistic to fund, implement, and sustain.
Core Technology
The BioButton System is a provider‑focused continuous monitoring platform that proactively collects and analyzes patient data to detect early signs of decline.

BioButton Wearable
Continuous vital sign and biometric measurements of patients both in facilities and at home
Flexible Gateways
Patient-Facing Mobile App or BioHub Cellular Gateway

BioDashboard Display
Exception Management Software to monitor patients in-hospital and/or home from a small office or command center
Rural Health Program Design
BioButton System Enables
Multiple Remote Care Applications
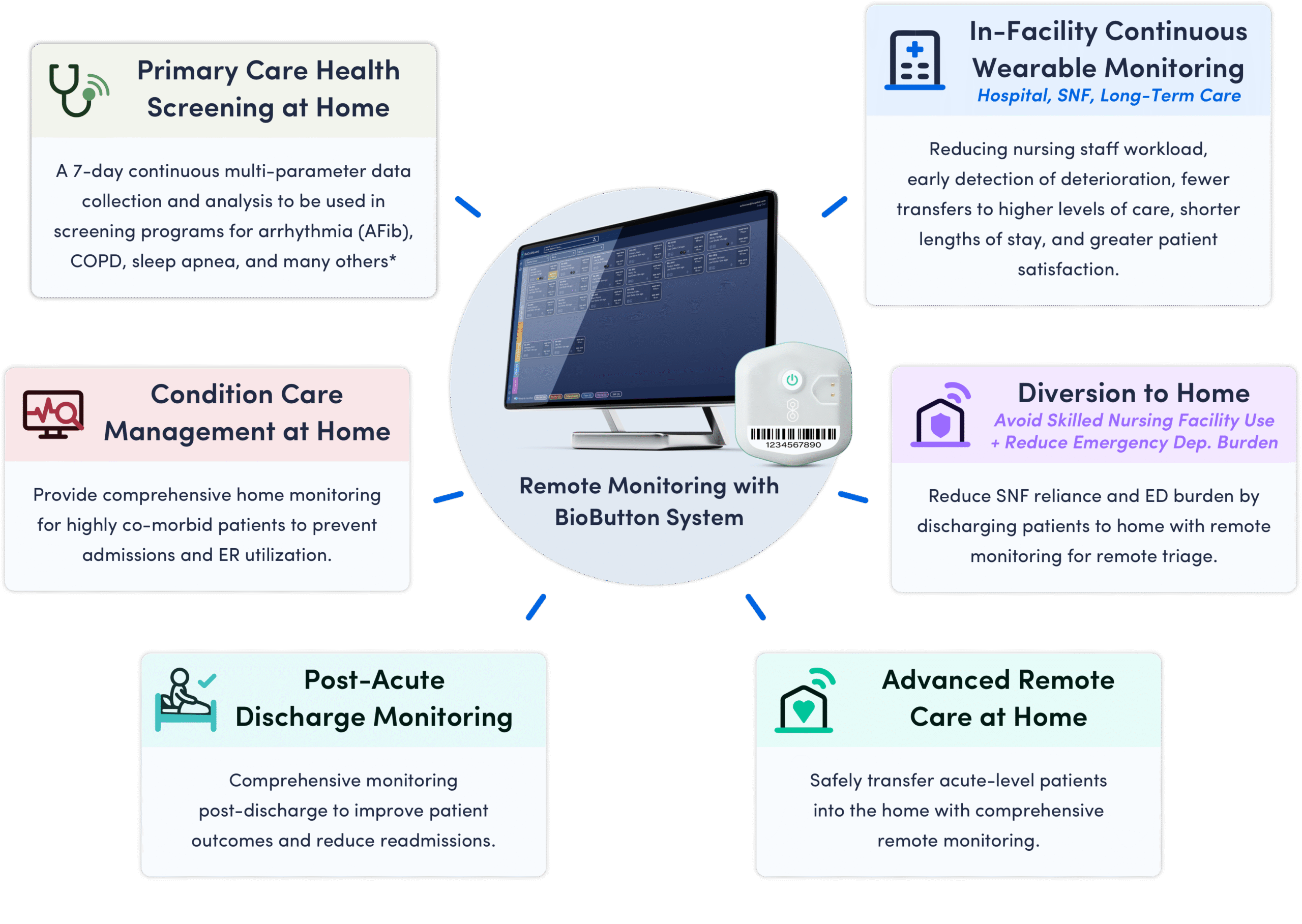

*Pending FDA clearance.
Condition Care Management Modules*
Acute + Complex Care Conditions
Chronic Stable Care Conditions
*Facility management and screening of specific diseases or conditions can be assisted by BioButton device monitoring and associated data. These claims are not within the intended use of the device as cleared by the FDA.
Anticipated Impact on Health Outcomes, Access, Quality, and Workforce Efficiencies
Continuous, multi-parameter monitoring has been shown to improve patient outcomes, expand access to care, and relieve pressure on rural facilities. BioIntelliSense translates this evidence into a rural‑ready program design that supports both clinical impact and operational sustainability.
Clinical + Care Outcomes
Continuous, multi-parameter monitoring programs have been associated with improvements in key clinical and access outcomes:
- Earlier detection of deterioration1-5
- Fewer readmissions and ED visits6,7
- Expanded reach into remote homes
Cost + Operational Benefits
These same programs also drive meaningful cost and operational benefits for rural facilities:
- Shorter length of stay and better bed utilization4,5
- Avoided transfers to higher level of care1-4
- Staff efficiency and burnout reduction7
Workforce Efficiencies in Moving From Manual Vital Signs to Automated, Wearable‑Based Continuous Monitoring
Continuous monitoring reduces repetitive vital sign collection and allows clinicians to focus on patients who need attention most, while lowering per‑patient monitoring costs.
4-6 Manual Vitals per Day
Clinician Labor Rate ($): $80/hr = $1920/24hrs
Patients per manual vital signs clinician: 20
$1920/24hrs/20 Pts = $96/Pt/24hrs
$96/patient/day for 4-6 manual,
intermittent vital signs
BioButton Continuous Vitals
Clinician Labor Rate ($): $80/hr = $1920/24hrs
Patients per BioButton monitoring center clinician: 500
$1920/500 Pts = $3.84/Pt/24hrs + $6/24hr for BioButton System
~$10*/patient/day for continuous
patient vital signs monitoring
Contact Us for Our Rural Health Transformation Kit
Ready to transform care for your patients? Use the form to get support designing or responding to an RHT Letter of Intent (LOI) or Request for Proposal (RFP).
Tell us about yourself and we’ll take it from there!
Appendix A: Works Cited
- Eddahchouri, Y., et al. “Effect of Continuous Wireless Vital Sign Monitoring on Unplanned ICU Admissions and Rapid Response Team Calls: A Before-and-After Study.” British Journal of Anaesthesia, vol. 128, no. 5, 2022, pp. 857–863.
- Verrillo, Sue Carol, et al. “Using Continuous Vital Sign Monitoring to Detect Early Deterioration in Adult Postoperative Inpatients.” Journal of Nursing Care Quality, vol. 34, no. 2, 2019, pp. 107–113.
- Weller, Robert S., et al. “Evaluation of a Wireless, Portable, Wearable Multi-Parameter Vital Signs Monitor in Hospitalized Neurological and Neurosurgical Patients.” Journal of Clinical Monitoring and Computing, vol. 32, no. 5, 2018, pp. 945–951.
- Stellpflug, Courtney, et al. “Continuous Physiological Monitoring Improves Patient Outcomes.” American Journal of Nursing, vol. 121, no. 4, 2021, pp. 40–46.
- Sun, L., et al. “Clinical Impact of Multiparameter Continuous Non-Invasive Monitoring in Hospital Wards: A Systematic Review and Meta-Analysis.” Journal of the Royal Society of Medicine, vol. 113, no. 6, 2020, pp. 217–224.
- Cleland, John G. F., et al. “Noninvasive Home Telemonitoring for Patients with Heart Failure at High Risk of Recurrent Admission and Death: The Trans-European Network–Home-Care Management System (TEN-HMS) Study.” Journal of the American College of Cardiology, vol. 45, no. 10, 2005, pp. 1654–1664.
- Pedone, Claudio, et al. “Efficacy of Multiparametric Telemonitoring on Respiratory Outcomes in Elderly People with COPD: A Randomized Controlled Trial.” BMC Health Services Research, vol. 13, 2013, article 82.
COM-18451 Ver.1 | Published 2026-2